Bariatric Surgery Brisbane
Obesity has become one of the world’s most impacting health problems, with people looking for different ways to lose weight, have a smaller stomach and lose excess weight in a long term meaningful way. Recent advancements in Bariatric Surgery have increased the likelihood of successful and sustained, long term weight loss when accompanied by appropriate nutrition and exercise.
Whilst a healthy diet and exercise can help with obesity, there are some who need more help than others to shed excess weight and deal with the health issues that arise with obesity and the resulting negative health effects that can deeply impact a
person’s health and wellbeing for decades to come.
Unfortunately, weight gain is a part of life, however sometimes excessive weight loss goes beyond conventional means and may need to be helped along the way to tackle this problem with Obesity Surgery, thankfully there are options available to people who need that little bit of extra help in obtaining a healthy long term weight.
Bariatric Surgery.
There are numerous types of Bariatric Surgery available such as gastric sleeve surgery, adjustable gastric banding as well as numerous laparoscopic surgery and keyhole surgery. Bariatric surgery is surgery that affects the stomach, and how food is digested. The purpose of bariatric surgery is to shrink the stomach or to make it so that the amount of food eaten is, in some cases, drastically reduced to allow for weight loss. Below we will take a brief look at some of the most common types of Bariatric Surgery and what it entails.
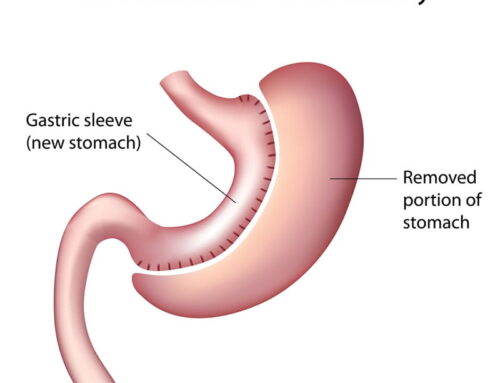
Gastric Sleeve Surgery involves the removal of a large portion of the stomach, including the part of the stomach responsible for Hormone Ghrelin or, the hunger hormone, this allows a person to feel fuller for longer, as well as removing the hormone that produces the feeling of hunger.
Hormone Ghrelin is responsible for the feeling of hunger, increases in food intake and also promotes fat storage throughout your body, once this hormone is effectively “turned off” by Gastric Sleeve Surgery, the body begins to become less hungry over time and lowers the amount of Hormone Ghrelin in your body, lowering the bodies want for food, it is one of the most effective treatments for chronic obesity.
Gastric Bypass Surgery involves creating a small stomach pouch that is stapled to the small intestine after some of the intestine has been removed, this allows for food to bypass most of the stomach, allowing for less calories to be absorbed by the stomach, with less calories and nutrients being absorbed, it leads to sustained weight loss by changing how much of your food the body absorbs and has the added bonus of keeping you feel more satiated as the pouch keeps food from being digested as quickly.
Lap Band Surgery involves a small adjustable ring made of salt water that is then placed around the top of the stomach that creates a small area where food is kept for longer in the top part of the stomach, it allows the patient to feel much fuller for much longer.
Lap Band Surgery is also known as laparoscopic adjustable gastric banding (LAGB), or gastric banding, once the band is in place it can be adjusted accordingly to accommodate less or more food throughout your weight loss journey.
Bariatric Surgery is an extremely useful procedure for those who have struggled with weight loss when conventional methods aren’t enough, or if their BMI is approaching or has reached a critical point, Bariatric Surgery is usually done as a keyhole procedure and has now become a standard operation for many countries
across the globe.
The benefits of Bariatric Surgery are now just limited to weight loss, it can also help to alleviate and help conditions caused by obesity that are often associated with higher body weights such as high blood pressure, diabetes, heart disease, stroke, sleep apnea, gout and many other “comorbidities’ often associated with high body weight and unhealthy nutrition.
Where to get Bariatric Surgery in Brisbane.
Dr Mastakov’s Surgery operates in 3 convenient locations across Greater Brisbane, Sunnybank, Cleveland and Hervey Bay, these practices offer most Bariatric Surgeries including Gastric Sleeve Surgery, Lap Band Surgery, Gastric Bypass Surgery as well as specializing in Weight Loss Surgery.
Dr Mastakov is a General Surgeon with over 26+ years of surgery experience, he is currently practicing at Mater Private Hospital Redlands, Sunnybank Private Hospital and, St Stephens Hospital, Hervey Bay.
For more information on this and more of the surgeries available at Dr Mastakov’s Surgery or for any enquiries, questions and available appointments, please visit https://mastakovsurgery.com.au/